Article
User Centered Design Is Dead
A 5-step rescue plan: modernize your product development process to design beyond the user.
A 5-step rescue plan: modernize your product development process to design beyond the user
User centered design is dead. Yes, I said it. And I meant it.
It’s not that I’m anti-user, of course. User centered design is critical to the success of most—if not all—products. Which is why we at M3 obsess over user needs every day. What kind of product developers would we be if we didn’t?
But it’s not all we obsess over. Because the user is just one piece in a large and complicated puzzle. The other pieces are made up of the many stakeholders that contribute to a product’s ultimate success—from caretakers to decision makers, retailers to manufacturers.
If anyone in the chain has a poor experience, your product’s success is at risk. This is particularly true in the case of high-value, complex systems, where many different stakeholders must successfully interact with your product for it to truly succeed.
And only one of these stakeholders is the user.
So let’s stop ignoring everyone else, shall we? In fact, let’s start a battle: user centered design versus stakeholder-centered design. Kind of like 20th-century-design-with-blinders-on versus 21st-century-design-that-actually-makes-sense.
In other words, our side’s gonna win. And it won’t be close. We’ll show you how.
Who the heck is this “user” in user centered design?
Let’s start with a couple of basic examples to compare user centered design with stakeholder-centered design. Exhibit A: that driving-you-to-distraction device in your pocket.
If you want to claim that a product’s end-user is the end-all, the smartphone is probably your best bet. Because in many (not all) cases, the end user is both:
• The one who makes the decision to purchase the product and
• Its sole user (save for when your 5-year-old steals it or your dog eats it)
So let’s say the smartphone manufacturer hones in on the user-centered goals of simple interactions and few user errors, focusing on:
- Superior affordance
- Intuitive interfaces
- Functionality that delights
In this case, assuming the thing works the way it’s supposed to, that it meets the business requirements necessary for making money, and that it is available to the desired markets, then focusing on user centered design could be enough to achieve success.
(Now, I’d argue that even in this case, you’d achieve a lot more success if you considered the other stakeholders as well, but for the sake of the comparison, I’ll leave it alone.)
But Who is the “User” of a Complex System?
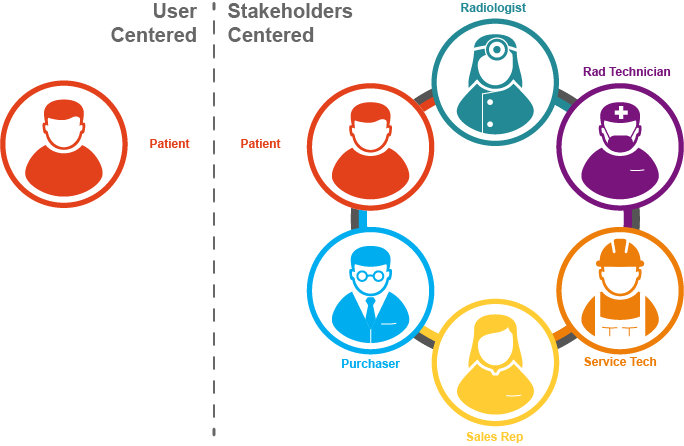
So what about more complex systems? Let’s look at an MRI diagnostic system for example. Focus on user centered design, you say? Okay, exactly who is the user?
Is it the technician who operates it every day?
Is it Fred, the frightened, claustrophobic, sensitive-to-noise patient who’s already panicked because of his medical condition?
Is it the radiologist who has to evaluate Fred’s MRI images?
Or is it the crew that installs and maintains it?
And let’s not forget the person who approved the system’s purchase in the first place. The all-important buyer.
So, user centered design soldiers, what say you? If you pick just one of these users, you fail.
If you choose the technician-operator, you might create a product that’s really easy to operate, but difficult to maintain and distressing for patients. So service-related issues will probably put the machine out of commission. Which might not matter much because patients will refuse to use the thing in the first place.
So, let’s design for that patient-user instead. That kind of feels right anyway, doesn’t it?
Great. Now you have a spacious, comfy solution for the patient. But it takes crappy images, is a bear to install, and costs three times as much as your competition. Say sayonara to your buyer.
To the victor go the winning products
If anyone in the chain of stakeholders has needs that are not adequately addressed, that oversight can prevent your product from being purchased and/or used to its utmost potential.
By limiting your thinking to a single user type, you don’t just limit your product’s potential success. You threaten to destroy that potential entirely, possibly before your product even reaches the ultimate user you designed it for.
The good news: It’s not that difficult to shift your point of view in this battle. And much of what informed your skill in user centered design will support your efforts in stakeholder-centered design as well.
So once you’ve jumped to the winning side, what’s next? It’s simple. Identify and understand everyone in your chain of stakeholders, then make sure all their needs are met, so that you keep that chain intact.
Let’s dig into it a bit more.
5 steps to stakeholder-centered design (for winners’ eyes only)
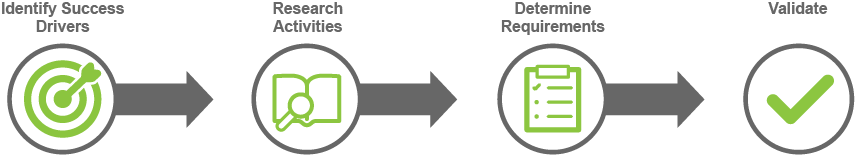
From the outset of your product-development project, you’ll use stakeholder-centered design to drive the following process. Each step guides the next:
- Identify critical success drivers
- Inform research activities
- Determine product requirements
- Validate product concepts & designs against requirements
Let’s unpack the process of understanding stakeholder needs and then integrating those needs into the product-development process.
Step 1: Map the Product Journey
First, map out every step your product will take from the point where potential purchasers become aware it exists until it is taken out of service and disposed of—beloved and well-used as it was. We refer to this sequence of steps as the product journey.
When you map this out, you’ll probably pinpoint 5 – 10 important steps. These steps will vary substantially based on your unique product and market.
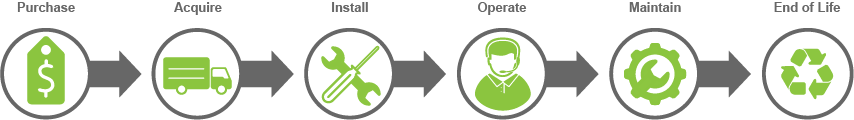
Steps in the product journey might include:
- Purchasing the product
- Acquiring the product
- Installing the product and bringing it online
- Using the product
- Maintaining and updating the product
- End-of-life actions
Step 2: Identify the Stakeholder List
Once you’ve created your product journey, you’re ready to roll up your sleeves and identify the many influential stakeholders who will affect success along the way.
Work through your journey map step-by-step, and identify every type of stakeholder who might influence the product’s ultimate success at each step.
Be sure to consider the following stakeholders along with any others that might be unique to your product:
- Intended users
- Unintended users
- User groups
- Purchasers
- Retailers
- Maintenance

Before calling your list a wrap, it’s helpful to check yourselves by asking some specific questions. For example:
- Who will interact with the product directly?
- Who will make the purchase decision?
- How is the purchase decision made?
- Who will install it?
- Who will operate it?
- Who will maintain it?
At this point, the goal is to identify as many types of stakeholders as possible.
Step 3: Map the Stakeholders to the Product Journey Steps
Next order of business: Create a user workflow diagram.
To do this, simply map your list of stakeholders to the product journey steps you outlined in step 1, specifying where each stakeholder fits in.
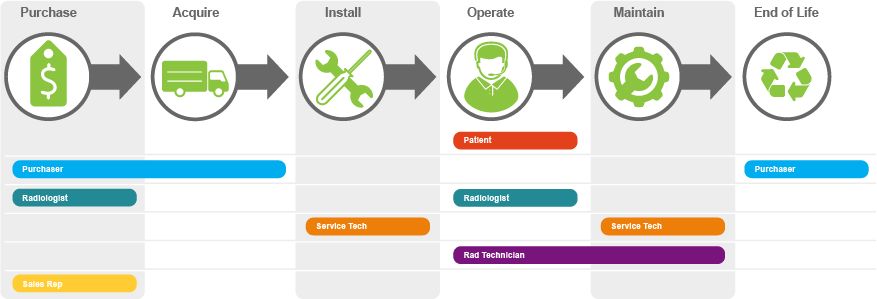
Hint: Keep in mind that most types of stakeholders tend to interact with the product at multiple stages in the product journey. That’s fine! At this point, your goal is simply to get all that recorded and clear.
Step 4: Identify What’s Important
Now it’s time to make sense of what you have.
The rubber meets the road during this step when you begin defining your critical success drivers. Your success drivers are the key indicators of what will make or break the product in the eyes of your stakeholders.
It’s important to acknowledge here that not all stakeholders and product journey steps are equal. So this is a time to leverage your best strategic minds to identify and hone in on the most essential items—those that you believe will make a difference in stakeholder outcomes or simplify stakeholder experiences.
Also, make sure that you’re focusing on success drivers that you can actually impact with design. I don’t care how gifted your creative team is; they can’t make a regulatory standard disappear!
Avoid focusing on that which you can’t change or that which has a negligible overall impact on outcomes. Instead, identify the items that appear to be most critical to the most important stakeholders. As you do, you’ll begin creating the list of success drivers that you’ll use to validate future product concepts.
Industry-specific tip: If you’re dealing with a medical product, remember your ultimate mission is to help achieve safety, efficacy, and improved patient outcomes. Medical products are unique in that every stakeholder shares that same ultimate goal.
Step 5: Use the Important Stakeholders as Research Targets
If you were formerly of the user centered design camp (until today, of course), then you already believe that you need input from the user in order to create your product design.
Stakeholder-centered design hinges on input as well. The difference is that we require input from all the key stakeholders rather than from a single type of user. So bonus! Now you have more types of people to learn from.

To gather information from the important stakeholders you’ve identified, perform whatever type of research is appropriate. This will support you in finalizing and validating your success drivers.
As you work through this process, keep an eye out for unintended users. When you discover them, update your user workflow diagram accordingly and adjust research activities as needed.
Remember, this is an iterative process. You should expect to uncover new questions along the way.
Design Your Products for all Stakeholders
Now you’re ready to wave the white flag on user centered design. By opening your eyes to the entire stakeholder chain, you reduce risk and boost your likelihood of product success immensely. Why would you do anything else?
You’ve got the tools, now get out there and delight your stakeholders!